Anterior Cruciate Ligament Reconstruction
What is the Anterior Cruciate Ligament (ACL)?
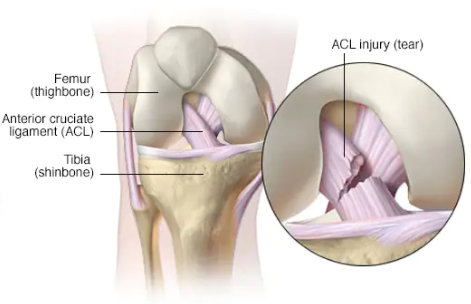
The Anterior Cruciate Ligament (ACL) is one of the major stabilising ligaments in the knee. It is a strong ribbon-like structure located in the centre of the knee, running from the femur to the tibia.
Unfortunately, when this ligament tears, it doesn’t heal and often leads to instability in the knee.
What Does the ACL Do?
The ACL prevents the tibia (shin bone) from moving abnormally on the femur (thigh bone). When this abnormal knee movement occurs, it is referred to as knee instability, and the patient is aware of it.
Often, other structures such as the meniscus, the articular cartilage (lining the joint) or other ligaments can also be damaged simultaneously as a cruciate injury. These may need to be addressed at the time of surgery.
- Most injuries are sports-related, involving a twisting injury to the knee.
- It can occur with a sudden change of direction, a direct blow, e.g., a tackle, landing awkwardly.
- Often, there is a popping sound when the ligament ruptures.
- Swelling usually occurs within hours.
- There is often the feeling of the knee popping out of the joint.
- It is rare to be able to continue playing sports with the initial injury.
What is ACL Reconstruction?
ACL reconstruction is a surgical procedure that aims to replace a damaged or torn ACL with a new ligament. In some cases, the new ligament is typically taken from other tendons of the patient's body or a donor. This surgery can now be performed with minimal incisions and low complication rates.
Who is Suitable for ACL Reconstruction?
If you have experienced an ACL tear or damage, and your symptoms have not improved with non-surgical treatments, you may be a good candidate for ACL Reconstruction. You may also be suitable for this procedure if you have a highly active lifestyle or participate in sports requiring sudden direction or pivoting changes. After a thorough evaluation and diagnostic testing, an orthopaedic surgeon can determine if ACL Reconstruction is the best option for you.
What are the Benefits of ACL Reconstruction?
There are several benefits of ACL reconstruction. Firstly, it can help to restore knee stability and function, allowing you to resume daily activities or sports without pain or discomfort. Secondly, it can prevent long-term complications such as arthritis or meniscus tears. Thirdly, it can improve your quality of life and overall well-being by reducing the risk of further knee injuries and the need for future surgical interventions.
ACL Reconstruction vs ACL Repair
Repair involves keeping the original ligament by directly suturing the two ends of the rupture together. Attempts at repair of ACL tears are now largely historical due to the high rate of failure of the surgery. However, advanced new techniques are showing promising results to allow repair rather than reconstruction in some cases. Better quality studies are still to come to support the repair techniques.
All ACL surgery nowadays is a reconstruction. This involves replacing the damaged tissue with a substitute tissue called a graft. The most commonly used grafts involve tissue from the patient (autografts). Tissue from donor patients (allografts) can also be used.
Types of ACL Reconstruction
- Autograft Ligaments
- Donor (Cadaver) Ligaments
Autograft Ligaments
The most commonly used autografts are
- Hamstring tendons
- Patella ligament
- Quadriceps tendons
There are pros and cons for each option. All three options are suitable and are associated with good results.
Cadaver Ligament
There are pros and cons of using cadaver tendons.
Pros
- Readily available
- Less painful operation with quicker recovery (because your tissue is not harvested)
Cons
- Tiny risk of infection
- Takes longer for the graft to incorporate
- Has a potentially higher failure rate than using your tissue
Essentially, allografts are options when there is no viable autograft (own patient tissue) to be used, such as multiple previous surgeries and usage of autograft prior.
Preoperative Preparation
Before undergoing ACL reconstruction surgery, you should undergo several tests to assess the extent of the injury and determine the best course of treatment. These tests include a physical examination, X-rays, MRIs, and blood tests. Your surgeon will also review your medical history and provide pre-operative instructions, such as avoiding food and drink for a certain period before the surgery.
ACL Reconstruction Procedure
Surgery is performed as a day procedure or overnight stay.
The surgery usually takes between 60–90 minutes.
Surgical techniques have improved significantly over the last decade, complications are reduced, and recovery is much quicker than in the past.
The surgery is performed arthroscopically.
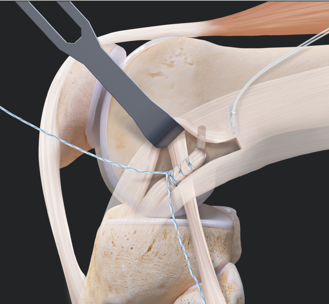
- The ruptured ligament is removed, and tunnels (holes) in the bone are drilled to accept the new graft.
- This graft, which replaces your old ACL, is taken from the hamstring or quadriceps tendon. Your doctor will discuss these options with you before surgery, based on your re-injury risk profile, level of activities and sports played.
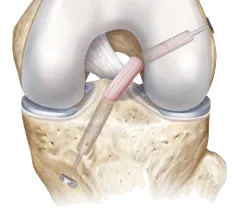
- The graft is prepared to take the form of a new tendon and passed through the drill holes in the bone.
- The new tendon is then fixed into the bone with various devices to hold it while the ligament heals into the bone (usually six months).
- The rest of the knee can be visualised simultaneously, and any other damage is dealt with, e.g. meniscal tears.
- The wounds are then closed, and a dressing is applied.
What is Adjuvant Extra-articular procedure or Lateral Tenodesis?
Lateral tenodesis consist of an extra-articular procedure performed in some cases where the Antero-Lateral Ligament (ALL) is suspected to be torn, as well as the ACL. This ligament has been shown to contribute to anterolateral instability, mostly seen when the ACL is torn in some cases, depending on physical examination.
Lateral tenodesis consist of an open procedure performed to a small 5-10 cm incision on the lateral aspect of the knee. The IlioTibial Band (ITB) is used as a graft to augment the deficient ALL and to improve rotational stability and outcomes.
Recent High-Level literature has demonstrated that the Extra-articular procedures improved stability, patient-reported outcomes and 3x reduction in the risk of graft re-rupture.
Lateral tenodesis is indicated for some patients with increased risk of graft re-rupture after ACL reconstruction, such as
- Patients involved in competitive/professional level of contact sports
- Under the age of 20 years old
- Revision surgery cases
- Patients with ligamentous laxity or with increased tibial slope
Ask your surgeon if you would benefit from Extra-articular procedures / Lateral tenodesis
Post-operative Recovery
See link attached for full ACL Rehab Protocol.
Pain Management
You will have pain medication by tablet or in a drip (intravenous).
A splint is sometimes used for comfort.
Wound Care
Leave any waterproof dressings on your knee until your post-op review.
- You can put all your weight on your leg.
- Avoid any anti-inflammatory or aspirin for ten days.
- Put ice on the knee for 20 minutes, as frequently as possible.
Post-op review
The first review will usually be after 10-14 days.
Physiotherapy
You will be seen by a physiotherapist who will teach you to use crutches and show you some simple exercises at home.
Exercise and therapy can begin after a few days or be arranged at your first post-op visit.
Complications
If you have any redness around the wound or increasing pain in the knee, or you have a temperature or feel unwell, you should contact your surgeon as soon as possible.
Why is Rehabilitation for ACL Reconstruction Essential?
Physiotherapy is integral to the treatment and should start as early as possible. Pre-operative physiotherapy helps prepare the knee for surgery better. The early aim is to regain range of motion, especially your full extension, reduce swelling and achieve full weight-bearing.
The remaining rehabilitation will be supervised by a physiotherapist and involve bike riding, swimming, proprioceptive exercises and muscle strengthening. Cycling can begin at two months; jogging generally begins at around three months. The graft is strong enough to allow sport at around six months. However, other factors come into play, such as confidence, fitness and adequate training.
Professional athletes often return at six months, but recreational athletes may take 10 -12 months, depending on motivation and time put into rehabilitation.
The rehabilitation and overall success of the procedure can be affected by associated injuries to the knee, such as damage to the meniscus, articular cartilage or other ligaments.
Risks & Complications of ACL Reconstruction
Like any surgery, anterior cruciate ligament reconstruction has risks. Some of the potential complications include
- Infection,
- Blood clots,
- Nerve damage,
- Graft failure,
- Knee stiffness,
- Chronic pain.
The risk of complications is generally low, and most patients experience a successful outcome. However, it is essential to discuss the risks and benefits of the surgery with an orthopaedic surgeon before deciding to undergo the procedure.
Prognosis of ACL Reconstruction
The prognosis of ACL reconstruction is generally good, with a success rate of over 90%. Most patients experience significant improvement in knee function and return to their regular activities or sports within six to twelve months after surgery. However, the success rate depends on various factors, such as the extent of the injury, the age and activity level of the patient, and adherence to post-operative rehabilitation protocols.
What if ACL Reconstruction is Delayed?
If ACL reconstruction is delayed, it can increase the risk of further knee damage and long-term complications such as arthritis and meniscal tears. Delayed surgery can also lead to prolonged recovery times and reduced knee function. In some cases, the damage may be irreparable, and the patient may require more extensive surgery or permanent knee bracing. Therefore, seeking prompt medical attention and following the recommended treatment plan is essential.