Collateral Ligaments Reconstruction
What are Collateral Ligaments?
Collateral ligaments are a pair of strong, fibrous bands of tissue that run along the sides of the knee joint. The knee has two collateral ligaments: the medial collateral ligament (MCL) and the lateral collateral ligament (LCL).
The MCL is inside the knee joint and connects the thigh bone (femur) to the shin bone (tibia). The MCL helps to prevent the knee from bending inward and provides stability to the inner part of the knee joint. The MCL can be torn with the Postero-Oblique Ligament (POL), and sometimes this ligament needs to be addressed in eventual reconstruction.
The LCL is outside the knee joint and connects the femur to the smaller bone in the lower leg (fibula). The LCL helps to prevent the knee from bending outward and provides stability to the outer part of the knee joint. Frequently the LCL is torn with structures of the Posterolateral Corner (PLC), and they need to be addressed in eventual surgical reconstructions.
What is Collateral Ligaments Reconstruction?
Collateral Ligaments Reconstruction is a surgical procedure that aims to replace damaged ligaments in the knee joint. The collateral ligaments are essential in stabilising the knee joint and preventing excessive movement that can lead to injury. Injuries to the collateral ligaments can occur due to sports injuries, falls, or other traumatic events.
During the surgery, the orthopaedic surgeon will make an incision on the side of the knee and will then use a tendon graft to replace the damaged collateral ligament. The graft is usually taken from the patient's body or a donor.
Who is Suitable for Collateral Ligaments Reconstruction?
Patients who have sustained injuries to the collateral ligaments in their knee joint are suitable for Collateral Ligaments Reconstruction surgery. In addition, patients who have chronic instability or dislocation of the knee joint may also be ideal for surgery.
Benefits of Collateral Ligaments Reconstruction
The main advantage of Collateral Ligaments Reconstruction is that it helps to restore stability to the knee joint. This can help to reduce pain and improve function in the joint. In addition, the surgery can help to prevent further damage to the joint and reduce the risk of developing osteoarthritis.
Patients who undergo Collateral Ligaments Reconstruction may also experience an improvement in their overall quality of life, as they may be able to return to their normal activities without pain or discomfort.
Types of Collateral Ligaments Reconstruction
There are several different types of Collateral Ligaments Reconstruction surgery, including
- Primary Repair: In some cases, the orthopaedic surgeon may be able to repair the damaged collateral ligament without the need for a graft.
- Autograft: An autograft involves taking a tendon graft from the patient's body, usually from the hamstring or patellar tendon.
- Allograft: An allograft involves using a tendon graft from a donor.
- Synthetic Graft: A synthetic graft uses an artificial material to replace the damaged collateral ligament.
The type of surgery used will depend on the severity of the injury, the patient's medical history, and other factors.
Preoperative Preparation
If you have been advised to undergo Collateral Ligaments Reconstruction surgery, there are several things you can do to prepare for the surgery and improve your chances of a successful outcome. Here are some tips to help you prepare:
- You will need to arrange transportation to and from the hospital, as you may be unable to drive after the surgery. You may also need assistance with daily tasks such as cooking, cleaning, and personal care, especially in the first few days after the surgery.
- Follow the specific instructions your surgeon provided on preparing for the surgery. This may include instructions on fasting before the surgery, stopping certain medications or supplements, and other pre-operative preparations.
- Get in good physical shape before the surgery, as this can help to improve your recovery and reduce the risk of complications. You may be advised to engage in low-impact exercises like swimming or cycling to improve your cardiovascular fitness before the surgery.
- Smoking can interfere with the healing process and increase the risk of complications after the surgery. If you are a smoker, quitting smoking six weeks before the surgery is essential.
- Eat a diet rich in protein, vitamins, and minerals in the weeks leading up to the surgery. A healthy, balanced diet can help to improve your immune system and promote healing after the surgery.
- You will need to prepare your home for recovery after the surgery. This may include creating a comfortable space to rest, stocking food and supplies, and arranging any necessary equipment, such as crutches or a knee brace.
Collateral Ligaments Reconstruction Surgery
Anaesthesia:
Before the surgery, you will be given anaesthesia to ensure you are comfortable and pain-free. Depending on your medical history and the surgeon's preference, you may receive either general or regional anaesthesia.
Incision:
Once you are under anaesthesia, the surgeon will make an incision on the side of the knee, exposing the damaged collateral ligament.
Removal of the Damaged Ligament:
The surgeon will remove the damaged collateral ligament from the knee joint.
Preparation of the Graft:
The surgeon will prepare the graft by taking a small piece of tissue from another part of your body or a donor. This tissue is usually taken from the hamstring tendon or allograft sources.
Placement of the Graft:
The surgeon will then place the graft into the knee joint and use screws and adjustable suspensory devices to secure it.
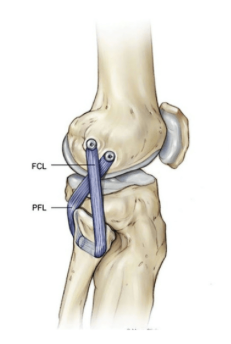
Graft configuration for an LCL and posterolateral corner (PLC) reconstruction.
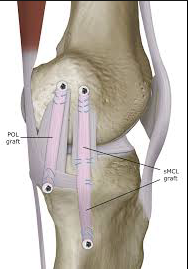
Graft configuration for an MCL and POL reconstruction
Closing the Incision:
Once the graft is in place, the surgeon will close the incision with stitches.
After the Surgery
You will be taken to a recovery room where you will be monitored closely for any complications. You will be given pain medication to manage discomfort and advised on caring for the surgical site. You will also be given exercises at home to help speed up the recovery process.
Post-surgery Care Instructions
Following Collateral Ligaments Reconstruction surgery, following your orthopaedic surgeon's post-surgery instructions is essential to ensure proper healing and a successful outcome. Here are some standard post-surgery instructions you may be given:
- You will need to rest and elevate your leg for the first few days after the surgery. This will help to reduce swelling and promote healing. You may be advised to keep your leg above your heart as much as possible.
- You will need to apply ice to the surgical site for 20-30 minutes at a time, several times a day, for the first few days after the surgery. This will help to reduce pain and swelling.
- You will be prescribed pain medications to manage discomfort after the surgery. You should take these medications as prescribed by your surgeon.
- You may need to wear a brace to help support your knee and reduce swelling. You will be instructed on properly applying and wearing the bandage or brace, usually for the first six weeks. Depending on each case, your surgeon will advise if the brace should be locked or unlocked to allow some range of motion.
- You will work with a physiotherapist to help regain strength and mobility in your knee joint. You will be given specific exercises at home and may need to attend regular physiotherapy appointments.
- You must attend follow-up appointments with your surgeon to monitor your progress and ensure proper healing. Your surgeon will advise you on when to schedule these appointments.
- You must avoid certain activities that could stress your knee joint, such as running or jumping, for several weeks or months after the surgery. Your surgeon will advise you on when it is safe to resume these activities.
Physical Therapy
In the weeks and months after the surgery, you will work with a physical therapist to help regain strength and mobility in the knee joint. Your physical therapy program will be tailored to your specific needs and designed to help you achieve the best possible outcome from the surgery.
Collateral Ligaments Reconstruction Prognosis
The prognosis for Collateral Ligaments Reconstruction is generally good. Most patients can return to normal activities within 6-9 months after the surgery. However, the recovery time may vary depending on the severity of the injury, the type of surgery performed, and the patient's overall health.
Patients who undergo Collateral Ligaments Reconstruction may experience an improvement in their overall quality of life, as they may be able to return to their normal activities without pain or discomfort.
Collateral Ligaments Reconstruction Risks
As with any surgical procedure, there are risks associated with Collateral Ligaments Reconstruction. Some of the potential risks include
- Infection,
- Blood clots,
- Nerve damage
- Anaesthesia complications,
- Failure of the graft.
You should discuss the risks and benefits of the surgery with your orthopaedic surgeon before deciding to undergo surgery.
What if Collateral Ligaments Reconstruction is Delayed?
If Collateral Ligaments Reconstruction is delayed, the patient may experience chronic instability or knee joint dislocation. This can lead to further damage to the joint and increase the risk of developing osteoarthritis.
Sometimes, if the ligament is only partially torn, non-surgical treatment options may be considered. These may include rest, ice, compression, elevation (RICE), physiotherapy, and pain medication.